Those N95 masks hurt.
To work, they must be worn tight. Within 20 minutes, the straps pinch your ears and the mask starts digging into your nose.
The masks need a tight seal to keep the coronavirus out. Doctors and nurses at Mount Sinai Hospital test their masks by reading aloud while saccharine is sprayed in their faces. If they taste sweetness through the mask, they’re dead — or they might be, if that mist were coronavirus droplets instead. Stubble on men can also throw off a mask’s fit.
Add goggles and gloves and hairnets and protective body coverings, then start treating a patient.
“It gets hot, it gets a little claustrophobic,” said Kimberly Lipetzky, a nurse at Mount Sinai. “I had a couple codes, doing CPR in full gear. Your goggles fog, and you’re trying to navigate this situation while of course performing at peak ability.”
“After an hour it starts getting really uncomfortable,” said nurse Adam Garrison. “It feels like the bridge of your nose is going to disintegrate.”
The COVID-19 crisis is gathering force in Chicago. Right now, infected patients still arrive at Mount Sinai, on Chicago’s West Side, in fits and starts.
“We’re definitely vacillating between moments of chaos and calm,” said Lipetzky. “Overall, there’s this heaviness, this weight in the air when you’re wondering, what’s going to come in the door? How do you be ready?”
In part by wearing two masks, layered, with donated, handmade cloth masks on the outside to protect the integrity of the vital N95 underneath. But that brings its own difficulty.
“It’s not exactly easy to speak,” said Garrison.
Which can impede the complicated, life-or-death communication that goes on in a hospital. A COVID-19 patient can deteriorate rapidly, can walk into the hospital in the morning complaining of shortness of breath and be on a ventilator by afternoon.
“I’ve never seen anything progress like this,” said Michele Mazurek, chief nursing officer for Sinai Health Systems.
To be put on a ventilator — a mechanical device that breathes for patients whose lungs are shutting down — a patient must be intubated: An endotracheal tube is put down their throat.
”Twenty milligrams of etomidate!” a doctor orders, her words muffled through the mask — etomidate, a short-acting anesthesia, knocks a patient out.
“Twenty milligrams of etomidate, correct?” the nurse repeats back, his words also muffled.
“Yes,” the doctor replies.
Hospitals call this “closed loop communication” — it makes sure patients are getting the correct drug in the proper amount at the right time.
“Twenty milligrams of etomidate being given in the right antecubital IV,” the nurse replies, “antecubital” being the medical term for the crook of the elbow.
Of people who get the coronavirus, 20% have no symptoms and might never know they had it. At the other end of the spectrum, 15% are so sick their lungs may start filling with fluid and begin shutting down. Breathing becomes short and rapid; the weakened body has difficulty drawing air. That’s why ventilators are so important — they force 100% oxygen into your lungs (regular air is 21% oxygen) and keep you alive as your body defeats the virus.
“Our main goal is to keep them oxygenated well enough that their body has a fighting chance to continue warding off the infection,” said Garrison.
All 21st century medicine can do right now is buy time.
“It’s all supportive care,” said Mazurek. “There’s no antibiotic, no antidote. To not be able to give something life saving ... it’s like strapping our hands behind our backs. It’s frustrating, not to save these lives, not to have an antibiotic. It’s a helpless feeling.”
There are a few drugs that sometimes help, like Remdesivir, an anti-viral used to treat Ebola. “That looks most promising,” said Garrison. “But it’s not an easy drug to get.”
Nor do they always work; Mazurek has watched a patient decline before her eyes. ”We have everything you can imagine at our fingertips,” she said “There’s nothing we could have done. We cannot stop the progression of this disease.”
After a car crash, a patient might be on a ventilator a few days. With COVID-19, patients could be on one for up to a month. This is why hospitals are scrambling to get more ventilators; they need so many because patients are on them for so long. Which itself leads to complications — pneumonia, skin breakdown, infection. Patients can survive COVID-19, then die from being on a ventilator.
This all happened so fast. The first COVID-19 patient was diagnosed at Mount Sinai two weeks ago this past Monday.
“At first it was a trickle,” said Garrison. “There has been exponential growth in the number of COVID-19 patients.”
Now, it’s a flood.
“These people coming in, they are sick, we’re admitting many of them,” said Dr. Sunita Mohapatra, head of infectious disease at Mount Sinai. “We’ve had to make a lot of changes to accommodate these patients. We have already filled our medical ICU, now taken over the surgical ICU, the trauma ICU. We’re not doing elective surgeries.”
“We’re at capacity,” said Michele Mazurek, chief nursing officer for Sinai Health Systems. “We feel the bell curve going up.”
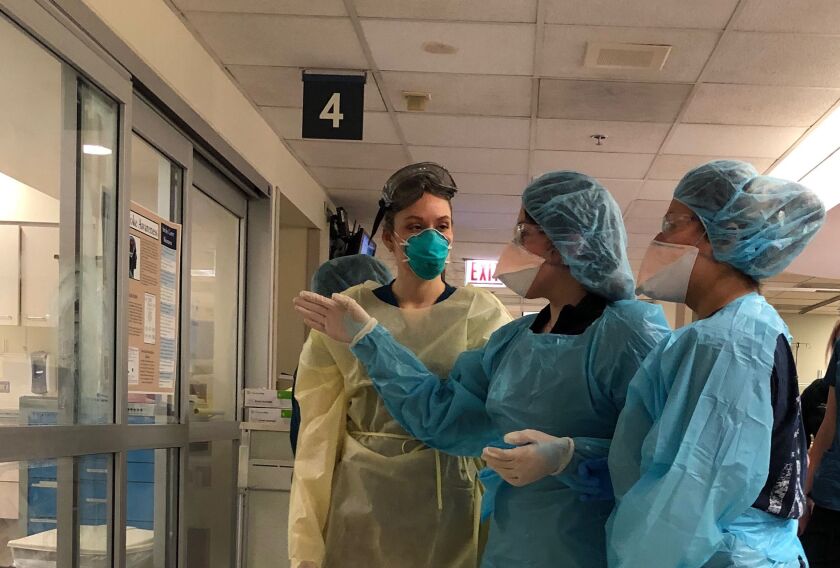
I’m focusing on Mount Sinai today and for the next two columns because I’ve spent time there previously, and some of their medical staff agreed to pause from the battle to save lives to answer questions. But this could be almost any hospital anywhere, in Chicago, the United States or the world. It seems to me we hear these terms — N95 masks, PPEs, ventilators — and see photos of medical personnel draped in blue without quite knowing exactly what is going on. I hope these columns help readers understand what is happening.
Thursday: A rapidly-escalating war