As a 52-year-old Galewood resident who lives alone and works outside, John doesn’t think he’s at high risk for getting COVID-19.
And with COVID vaccines only getting approval for emergency use by the federal Food and Drug Administratin less than six months ago, John doesn’t believe there has been enough time to determine if there will be long-term health impacts from getting a shot.
“I think I can avoid the virus, and I think my health factors indicate I would survive COVID,” said John, a landscaper who asked that his name not be used.
He’s not going to get the vaccine — at least not yet.
“I would like to wait until there is more data,” he said.
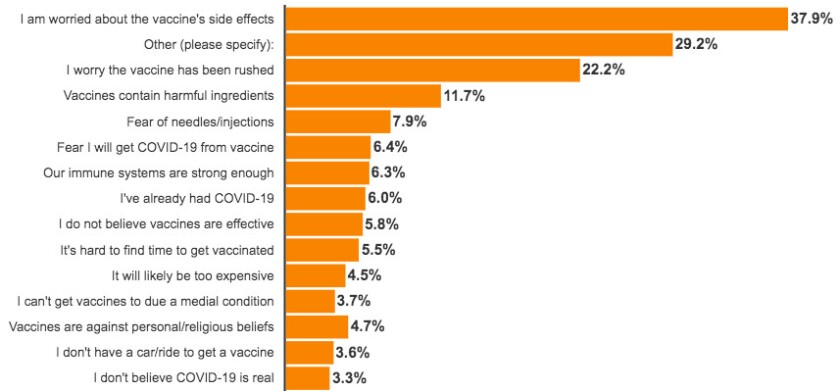
Fears of side effects from the shots remain the top reason Illinois residents reject the shots, new statewide polling data show.
That, as well as persistent worries the entire process to develop the vaccine was rushed — a concern John also shares — could have contributed to the slowdown in vaccinations that has hit the state in recent weeks, the data shows. About half of Illinois adults are now fully vaccinated, although experts say as many as 70-90% need to get vaccinated to reach herd immunity.
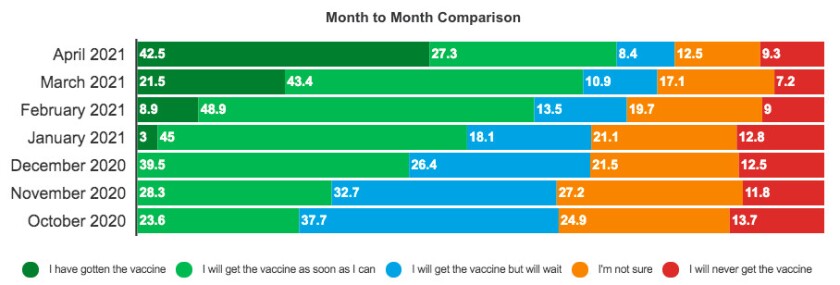
But the data released earlier this week show there is some progress, as only 38% of residents now worry about side effects, down from 53% in December. The number of Illinoisans who say they will never get a shot has dropped to 9.3% — a slight uptick from last month but down from 13.7% in the fall.
How likely are you to get the COVID-19 vaccine?
And when compared to neighboring states in the Midwest, the data show, Illinois now has fewer respondents who said they would never get a COVID-19 vaccine than Indiana (15.2%), Missouri (13.9 %), Iowa (11.7 %) and Michigan and Wisconsin (11.1 %).
The Illinois data comes from a monthly health survey of roughly 1,000 consumers by the National Research Corp. It highlights statewide vaccine-related concerns among residents every month between October and April.
In addition to side effects, an analysis of the data by the Documenting COVID-19 project at the Brown Institute for Media Innovation shows, many concerns linger as the vaccine rollout now enters a critical period toward reaching herd immunity.
About 22.2% of respondents continued to express the concern the vaccine’s development was rushed last month. Among Illinois Hispanics, the number who still think it was developed too quickly is 5 percentage points higher than the general public.
“We’re talking to people and they say things like, ‘I’m nervous about it, but I know I need to do it,’” said Shelly Ruzicka, spokeswoman for Arise Chicago, a faith-based nonprofit that advocates for workers’ rights, including for many Latino and Polish immigrants. She said fears have been expressed by residents and staff members alike even as the group has brought in health professionals for virtual Q&A sessions and provided vaccine information in multiple languages.
What concerns do you have about the COVID-19 vaccination? (Select all that apply)
Other concerns have resulted from differences in political beliefs or even misinformation that has spread rapidly online and elsewhere.
“There were a lot of fears of ‘the chip,’ or they’re being tracked,” Dr. Vidya Sundareshan, the medical adviser in downstate Sangamon County, said of false claims the vaccine contained microchips. “A lot of young women wanting to get pregnant, and in that age group, they would worry about infertility as a result of this vaccine.” Experts say there is no evidence vaccines cause infertility.
What’s more, between about 3-4% of people, dating back each month to November, have said they don’t believe COVID is even real.
“There are the political barriers, which I don’t remember ever having to face before,” Champaign-Urbana Public Health District Administrator Julie Pryde said. “People believe for some reason that it’s a government conspiracy.”
Sundareshan, who is also a professor of infectious diseases at the Southern Illinois University School of Medicine, said the concerns have contributed to a slowdown in vaccinations despite early progress in Springfield.
“We had come to a certain point, and that’s it, there was no movement after that,” she said.
Small numbers of respondents to the survey also listed more practical reasons for not getting a shot like not having time or a ride to get to a clinic.
More intensive community outreach is critical to countering vaccine hesitancy, said Dr. William Parker, an assistant professor of pulmonary critical care medicine who is assistant director for the University of Chicago MacLean Center for Medical Ethics. Many South Side neighborhoods not far from the university still have some of the lowest vaccination rates in the city.
“We need some convincing to remove as many barriers as possible,” Parker said.
Contributing: Manny Ramos
Kyra Senese is a reporter for the Brown Institute for Media Innovation’s Documenting COVID-19 project, a collaborative open-records journalism initiative made up of researchers from Columbia and Stanford universities.