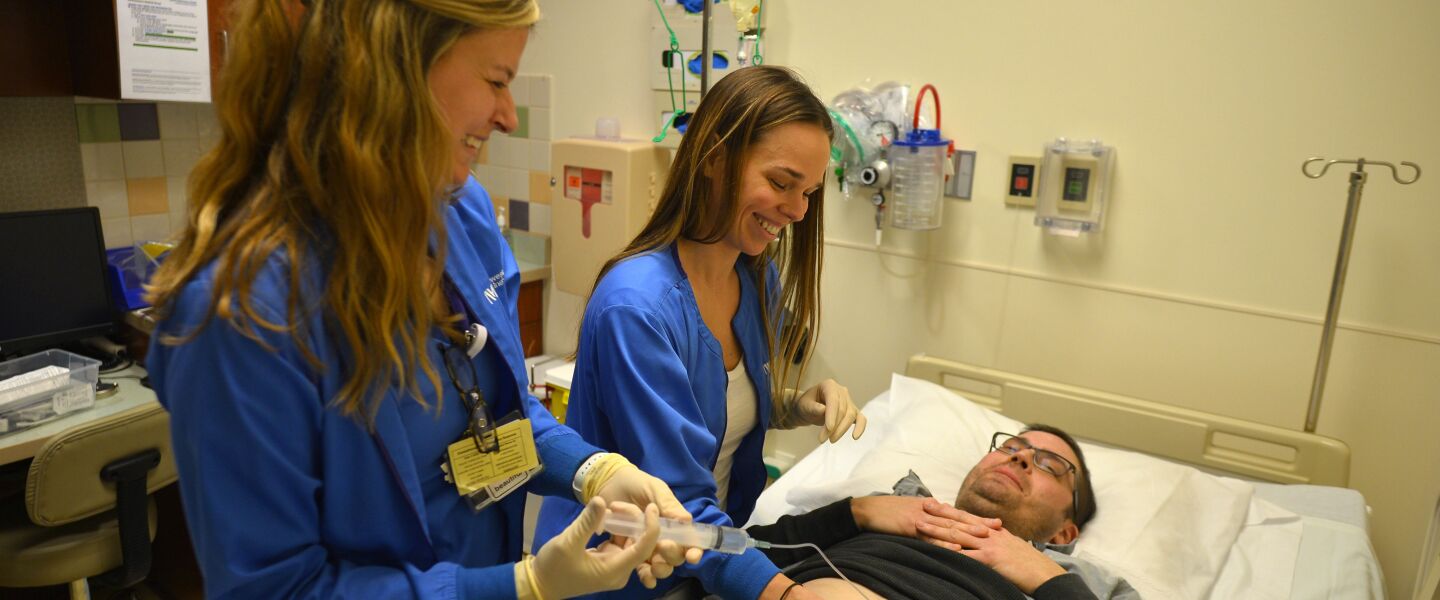
In August 2017, Shannon Harrity found out she was pregnant. Two days later, her husband Sean O’Reilly learned he had metastatic cancer. It had started years earlier in his colon, then spread to his liver.
O’Reilly’s previous doctors had puzzled over his stomach problems, his bloody stools. Maybe hemorrhoids, they speculated. He was so young — in his late 30s. Too young to bother with a colonoscopy. Too young to worry about what the NU doctors found — spreading colon cancer, Stage 4.
“You hear the ‘C-word,’ and you think it’s over, you’re dead,” O’Reilly says. “There is no Stage 5. You’re six feet under the ground.”
Chemotherapy started two weeks later. In a second irony, while he was back at Northwestern Memorial Hospital’s Lurie Comprehensive Cancer Center for his first chemotherapy session, as the virulent chemicals were dripping into his veins, his wife was across the street at Northwestern’s Prentice Women’s Hospital, learning she was carrying twins.
How does a couple respond to this kind of one-two punch?
“Happy but devastated,” says O’Reilly, an analyst for the federal government.
“A lot of life changes in very little time,” says Harrity, who works in human resources for a consulting company. “We were definitely overwhelmed.”
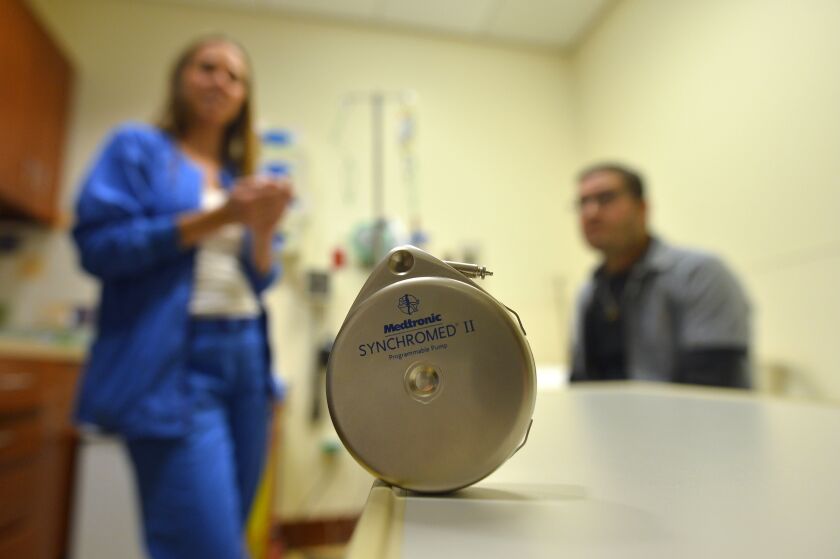
A hepatic artery infusion pump in Sean O’Reilly’s abdominal delivers high-dose chemotherapy directly to the liver through a large artery, the hepatic artery. O’Reilly (right) and oncology nurse Caroline Castino prepare for the procedure at the Robert H. Lurie Comprehensive Cancer Center of Northwestern University.
Victor Hilitski / Sun-Times
Even his doctors were moved.
“Emotional for all of us,” says Dr. Ryan Merkow, O’Reilly’s surgical oncologist. “It had a big impact.”
O’Reilly was 39 when he learned he had cancer, making him part of a new development doctors have identified but don’t yet fully understand. Colon cancer is down among older Americans — those over 50 — but up sharply among the young, jumping by 20%.
“We’re definitely seeing a trend here,” says Dr. Mary F. Mulcahy, O’Reilly’s medical oncologist. “Reports from across the United States show it is on the rise in people less than 50, on the decline in every other age group.”
Nobody knows why.
“Everyone wants to attribute it to the rotten American diet, but that isn’t it,” Mulcahy says. “This is across the world. Incredibly healthy people with incredibly health diets have it.”
“Probably a complex interaction with something in the environment,” Merkow says. “We have to assume it’s environmental, not from genetics.”
For O’Reilly, his youth made his diagnosis all the more stunning.
“When I was diagnosed. I was astounded,” he says. “It was shocking to me. ‘This is what old people get.’ Since my diagnosis, over the past two and a half years I have met more young people with colon cancer than older people with colon cancer.”
His wife wishes they had more aggressively pursued answers.
“Sean had symptoms for years,” says Harrity, crying. “He went to the doctor, time after time, and was told: It’s nothing, don’t worry about it. They were using language that made us believe they were taking this seriously. But they weren’t.
“This could easily have been caught much sooner, and it’s important that people know these types of symptoms. He was fatigued. He had blood in his stool. Several times he said, ‘Should I go have a colonoscopy?’ and the doctor said, ‘Don’t worry, it’s not necessary.’ ”
The good news was that, after two years, the tumors in his colon became so small as to be undetectable. But at least 10 tumors were growing on both sides of his liver. So many that they couldn’t be removed surgically.
“The surgery would damage too much normal liver,” Mulcahy says. “It does regenerate, but you have to spare an artery, a vein, a bile duct. If you’re taking out too large a section of the liver, it’s going to cause liver failure.”
Nor was a transplant an option. With liver cancer, the rate of recurrence is high: 50% that It could come back in the new liver.
And the immunosuppressant drugs that keep a body from rejecting a new liver undercut its ability to fight off cancer. Transplants have been given to people in O’Reilly’s situation. While his doctors say it isn’t in the cards, not now, he is hopeful.
“I like to think it’s still an option,” O’Reilly says.
With surgery and a transplant unavailable, all that was left was chemo. The problem, though, is that, in time, chemo — and he has had 70 rounds of it — begins to lose its efficacy. That happened to O’Reilly last year.
“We’d run of options,” Merkow says. “He’d been through every type of systemic chemotherapy. Its ability to control his liver disease was becoming less effective.”
Merkow decided to try a treatment that has fallen out of general use but with new types of anti-cancer drugs is being revived as a way to concentrate the chemo directly at the site of the cancer.
“The hepatic artery infusion pump has been around for several decades, since the 1980s, and gone in and our of favor,” Merkow says. “It’s not commonly used now — there are three or four hospitals in the Midwest using it. We’re the only ones in Illinois.”
In May, 2019, Merkow implanted the pump, which is about the diameter of a hockey puck though thankfully a bit thinner, in O’Reilly’s abdominal wall, with a catheter going directly into the artery feeding the liver (hepatic means relating to the liver).
His gallbladder was in the way, so it as removed — you don’t really need one. The two milligrams of daily chemo goes directly into the liver, where it stays, attacking cancer cells.
“Putting the pump in, we can have higher doses, more intensive therapy,” Merkow says. “The drug is completely metabolized in the liver, so there really are no side effects from chemotherapy.”
Every two weeks, O’Reilly, who lives in the South Loop, goes to Northwestern to receive systemic chemo to keep the cancer from taking hold in the rest of his bod, and to have his pump filled either with chemo or a saline solution to keep the lines clear while allowing the liver to rest. But lately the tumors are growing again — a setback — and a week ago the pump was filled with chemo again.
The goal now isn’t to cure the cancer so much as to live with it as long as possible.
”We’ve achieved disease control,” Merkow says. “He’s had a very good response. In these situations, where we can’t remove everything, we convert it into a chronic disease, trying to achieve the beset possible outcome.”
“He’s likely to be on treatment indefinitely,” Mulcahy says. “This therapy is buying us time. He’s living with cancer. He’s doing well. It’s a lot — for him and his wife and his kids. It’s a hard life, to live with cancer.”
But live they do, lives that — though it sounds strange to say — are, in a sense, enriched by the cancer. O’Reilly journals about his battle.
“You want to be aware of what your thoughts are,” he says. “There’s value in suffering. It gives you exposure to another element of human existence yo wouldn’t have otherwise had.”
O’Reilly hasn’t missed a day of work. His twins Madelyn and Vivian are now almost 2 — one named for a particularly friendly staffer at Northwestern — and are “curious and rambunctious girls.” The couple’s son Eamon, who was talking in full sentences at 2, is now 6 and keeps track of his father’s struggle.
“He knows his father has cancer and it sometimes makes him tired,” Harrity says.
Some parents are so busy they aren’t present with their young children. O’Reilly’s experience is the opposite. Living perhaps on borrowed time encourages him to focus on the living part and not on the time.
“In a way, it’s a blessing,” he says. “Because you are living a life so much deeper than it ordinarily would have been. When you’re living in the present more, you really understand and value every moment you have with your children. You’re not taking them for granted. You are living in the here and now.”
“We hope there’s an end, but we’ve been at it a long time,” Harrity says. “I’m the emotional one ... Who wouldn’t be? He is incredible, always one step at a time. It’s not about what happens to you but how you respond. He’s resilient, and he is responding better than a lot of people in his situation would. We’ve been very happy.”
“I became very depressed for three to five months,” O’Reilly says. “I did a lot of reading, thought a lot about choice. It’s my decision to be positive or negative. The negative road leads nowhere. All successful stories deal with positivity. Science reflects that the human body heals ridiculously well with positivity. It actually affects cells and healing. That’s why people who are stressed get sick.
“At the end of day, all you have is a decision. You either push things away and resist. Or you accept and embrace. Like anything in life. I decided to accept it and embrace it. Because the other decision leads nowhere. Negativity leads nowhere. There’s freedom in embracing and acceptance.
“I don’t view this as a death sentence anymore. I view it as: I’m going to beat it, or I’m going to live with it.”