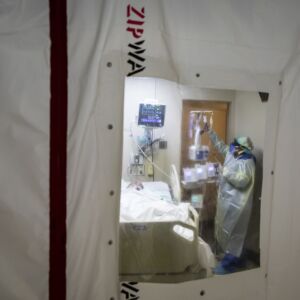
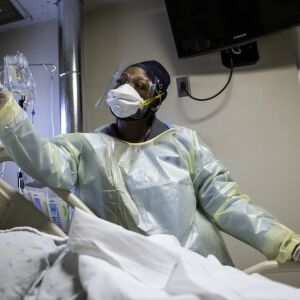
Look closely, through the face shield, over the mask. You’ll see it.
“Walk around the hospital, you can see the fatigue in people’s eyes,” said Dr. Roy Werner, director of the emergency department at Roseland Community Hospital on the Far South Side. “We have an entire staff of physicians, nurses, tech staff, housekeepers, working harder than they have ever had to work.”
Eight months into the COVID-19 pandemic, with a vaccine tantalizingly near but still not in hand, the relentlessness of fighting the virus — the endless stream of patients, the round-the-clock shifts, the deaths, the need to plug holes in the schedule created by sick colleagues — is grinding down hospital workers.
Werner said “close to 50, 60 percent” of emergency room staff at Roseland already have contracted the coronavirus, including himself. Many still battle it while colleagues struggle to carry the load. That’s true across the city.
“You can’t take vacation, you can’t escape at work,” said Dr. Meeta Shah, an emergency room physician at Rush University Medical Center on the Near West Side. “Sometimes you can’t escape in your sleep. There is an overall fatigue, not being able to get the break we need. That can be exhausting.”
A Chicago Medical Society poll of its 17,000 members shows two-thirds report symptoms of burnout: physical and mental exhaustion, listlessness. emotional numbness. And that was over the summer.
“It’s worse now, because everybody is busy all the time,” said Dr. Vishnu Chundi, chairman of the COVID-19 Task Force for the CMS. “There’s no letup.”
Chundi said not only are doctors overworked, but more are coping with their own post-COVID-19 symptoms — shortness of breath, chronic pain.
“Now we’re seeing more of the staff getting it,” he said. “They’re not having enough time to recover from COVID — the fatigue, the cough. They’re coming in ragged around the edges.”
When they do, they face patient death on a scale they are simply not used to.
“It’s horrible,” Chundi said. “I’ve never seen so many people die. It’s just a number until you see it happen in front of you. Then it’s, ‘Oh my God — this is carnage.’”
Despite the vaccine, the pandemic will rage at least until April, he said: “You’re going to see half a million people dying in this country.”
Until then, it can be a struggle for doctors to keep up with medical research, like playing a sport where the rules and equipment keep changing mid-game.
“I’ve never lived through anything like this,” said Dr. Mark Yoder, medical director of the Medical Intensive Care Unit at Rush. “Medical evidence just bombards you. Search medical papers; there are 60,000 articles on COVID published in the last year. I try to keep up. But I can’t read 60,000 articles.”
“The science itself is fluid,” said Shah. “Therapies continue to change. It can be quite confusing.”
“Something can look promising, using the research methodology from one country, one group, one hospital,” Yoder said.
“Then science finds out about it and debunks it: ‘No, that doesn’t work,’” he added. “We’re seeing things coming into vogue, being done, then being disproved. People were so convinced hydroxychloroquine was the answer and it was saving lives. Now so many trials show it’s absolutely worthless and should not be used because it can harm people.”
The type of patient has changed too.
“The first wave, we had people who have lots of other illness — from nursing homes; on dialysis,” said Chundi. “Here we’re seeing grandma and grandpa, people who were previously doing OK. Wave after wave after wave.”
You can die of COVID-19 without having it
Much about this pandemic is counterintuitive.
COVID-19 kills patients who don’t even get it. How? Indirectly. They die of conditions that might have been dealt with successfully, except they feared entering a medical system overwhelmed by COVID-19.
“People who needed to come in, didn’t,” said Yanina Purim-Shem-Tov, vice chair of faculty development and research for the department of emergency medicine at Rush. “Patients coming in with heart attacks, strokes, all those were delayed. Patients were afraid of coming into the hospital.”
Ironically, while patients worry about going to hospitals because of COVID-19, hospital staff suspect they’re getting sick — not by working 12-hour shifts in an emergency room, where precautions are taken, but at home.
“The staff are not necessarily worried about getting COVID at work,” said Shah. “You go out somewhere just for an errand. Someone comes to work at your home. I don’t walk around with a face shield on 24 hours a day. Sometimes I think I’m safer in the hospital despite the fact I’m seeing all these COVID patients all shift long.”
Not all news is bad.
“Here’s the good news: we seem to know more about what we’re doing,” said Shah. “There are more therapies out there. We are trying everything we can to utilize those therapies so patients don’t end up on ventilators. Some of the therapies, we feel more confident giving them. The safety profiles are more reliable, the impact more reliable.”
“We used to see information changing on a daily basis,” said Purim-Shem-Tov. “It’s stabilized now.”
“In the first wave, we found steroids were actually hurting patients,” said Werner. “Over the course of the last few months, the way the pandemic has moved across the world, we found very specific places, if steroids were given patients, the outcomes were astronomically better.”
In many cases, it isn’t the coronavirus per se wreaking the damage, but your body trying to fight the virus — particularly inflammation — by attacking itself: heart, liver, kidneys, lungs.
“The blood starts to clot in the little tiny vessels, causing organs to shut down, leading to death,” said Werner. “Steroids take that away, especially in the early, inflammatory stages.”
In the spring, the concern was getting enough ventilators to hospitals. Now doctors try hard not to use those ventilators.
“That’s where things have changed,” said Yoder, noting previously patients were put on ventilators sooner than necessary because doctors wanted to avoid having to do so quickly, under emergency conditions. “With COVID in the first surge, we were intubating people who didn’t need to be intubated. We were over-utilizing mechanical ventilation, just to be safe.”
“Patients with low oxygen levels, we used to intubate them right away, put them on a ventilator,” said Purim-Shem-Tov. “Now we try not to do that, instead using different modalities of oxygen delivery.” That cuts down on lung injuries caused by the ventilators, plus the complications from being sedated.
Caring for the caregivers
The Chicago Medical Society is so concerned hospital personnel don’t have anywhere safe to recharge they’ve begun a program with the Illinois Fitness Alliance, opening health clubs and gyms across the state for doctors and nurses to use, free, over the next few months.
“Get rid of stress, and put some normalcy and routine back into their lives,” said Chundi.
The CMS also helps members deal with an aspect that barely gets mentioned: doctors and hospitals are suffering financially. Lockdown dries up the demand for specialties such as orthopedics or dermatology, and a cratering economy undercuts elective surgeries.
“Some systems laid off a significant number of people, right after the first wave,” said Chundi. “Everything calmed down, and there was a workforce reduction. Now we don’t have those people.”
Meanwhile, specialties crucial to treating COVID-19 are in short supply.
“We have not had enough respiratory therapists,” said Yoder. “That’s true in hospitals across the country.” One 280-bed hospital in Chicago typically staffed with six respiratory therapists was getting by with three. The rest were out with COVID-19.
The pandemic has caused some doctors to retire, others to do mid-shift career changes, from specializing in neonatal/pediatric lung care to treating adults.
“Adult ICU patients are taking people a little out of their comfort zone,” said Yoder. “But fortunately they were trained in both pediatrics and adults, so there is tremendous flexibility.”
Asked what message is most important to get to the public, every doctor says a version of the same thing.
“Distance and mask. Please,” said Yoder. “The more you mask yourself and don’t gather into large settings, the better it is for all of us.”
“Listen to the people who know what they’re talking about,” said Werner. “The infectious disease people, like Dr. [Anthony] Fauci. This disease is real. This disease is killing our loved ones. It’s also killing our communities. Just listen. Put masks on. Listen to the pros.”
Contributing: Ashlee Rezin Garcia
Wednesday: How coming down with COVID-19 changed how one doctor views patients.